Key Takeaways
- Eating 30+ different plant types per week is one of the most evidence-backed ways to build a diverse, healthy gut microbiome.
- Fermented foods like yogurt, kefir, and kimchi have been shown to reduce inflammatory proteins and increase microbial diversity.
- Ultra-processed foods actively deplete your gut’s good bacteria cutting them is as important as adding healthy foods.
- Chronic inflammation quietly damages the gut lining, reduces microbial diversity, and drives conditions like IBS, obesity, and type 2 diabetes.
- Poor sleep and chronic stress disrupt the gut’s circadian rhythm, reducing microbial richness even in just a few nights.
- Regular moderate exercise increases short-chain fatty acid production, which protects and nourishes the gut lining.
- Gut health is built through daily consistency, not quick fixes small changes compound into real, lasting results.
What Is Gut Inflammation?
Gut inflammation is the immune system’s response to a perceived threat inside the gastrointestinal tract. In small doses, inflammation is protective it helps your body fight off harmful bacteria, viruses, and damaged cells. The problem begins when it becomes chronic and low-grade, meaning it stays switched on at a quiet but persistent level without a clear infection or injury to fight.
This kind of ongoing inflammation is increasingly common in modern life, and diet is one of its biggest drivers. When the gut lining is repeatedly exposed to harmful substances whether from ultra-processed foods, alcohol, stress hormones, or disrupted sleep it can become more permeable. This is sometimes described as “leaky gut,” a state where the tight junctions between intestinal cells loosen, allowing bacterial toxins and undigested food particles to pass into the bloodstream.
Once in the bloodstream, these particles trigger a systemic immune response. The body stays in a low-level state of alarm. Over time, this becomes the foundation for a wide range of chronic diseases.
How Inflammation Affects Gut Health
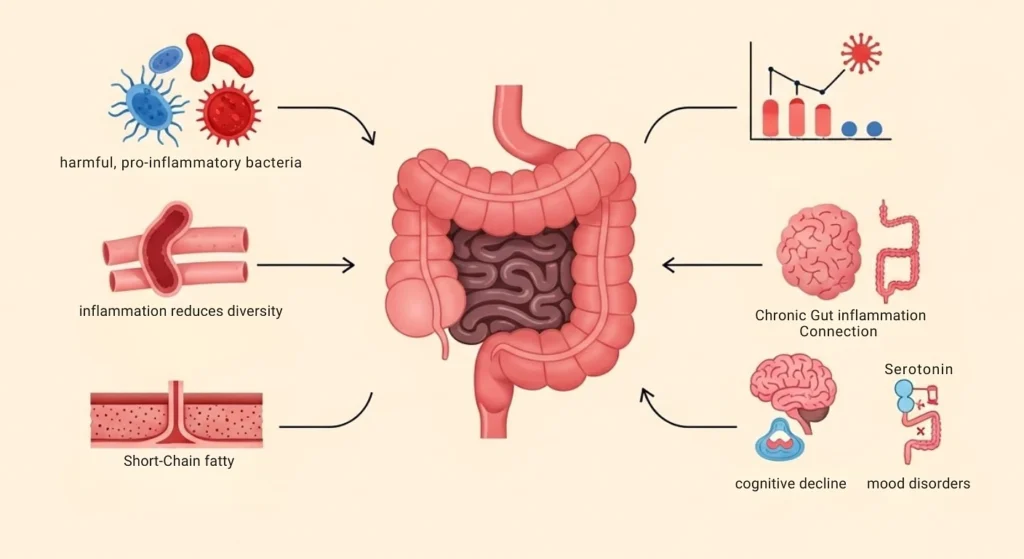
- It kills off beneficial bacteria. Inflammation creates conditions where harmful, pro-inflammatory bacteria thrive and protective species decline. Research published in Nutrients (2025) found that diets high in synthetic additives are associated with a drop in two of the gut’s most protective species Akkermansia muciniphila and Faecalibacterium prausnitzii both of which play a direct role in maintaining gut barrier integrity and reducing inflammation (Facchin et al., Nutrients, 2025).
- It reduces microbial diversity. A less diverse gut microbiome is a weaker one. Lower microbial diversity has been consistently linked to obesity, type 2 diabetes, inflammatory bowel disease, and even depression. The relationship is circular: inflammation reduces diversity, and lower diversity makes inflammation worse.
- It damages the gut lining. The gut barrier a single layer of cells separating your gut contents from your bloodstream depends on a healthy microbiome to stay intact. When beneficial short-chain fatty acid producers are depleted by inflammation, the cells lining the colon lose their primary fuel source, and the barrier weakens.
- It affects the brain. Through the gut-brain axis, chronic gut inflammation has been linked to mood disorders, cognitive decline, and anxiety. Around 90% of the body’s serotonin is produced in the gut, and inflammatory disruption to microbial balance directly affects this production.
How to Reduce Gut Inflammation and Improve Gut Health
1. Eat a Wide Variety of Plants
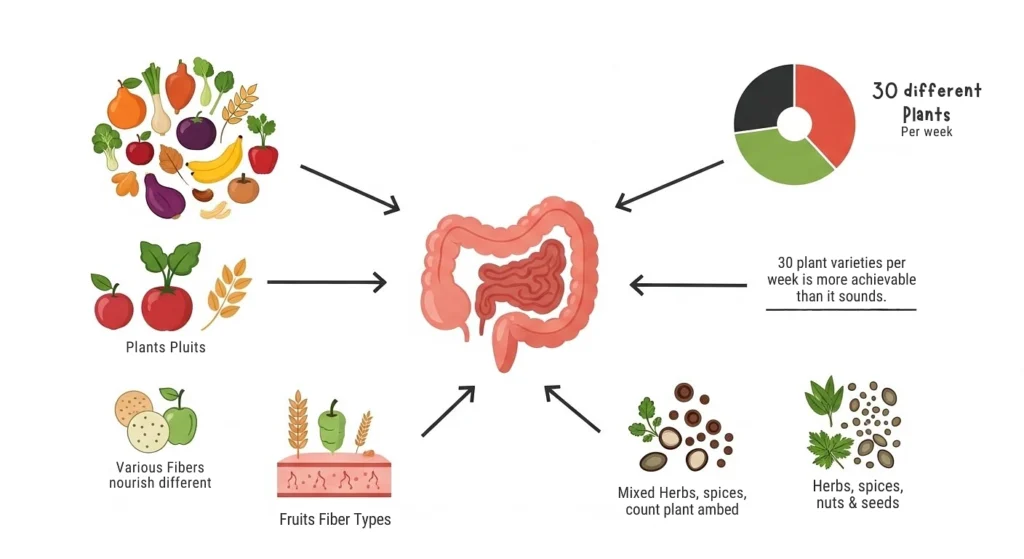
If there is one thing researchers have consistently found, it is that diversity in the diet creates diversity in the microbiome and a more diverse microbiome is a more resilient, less inflamed one.
The American Gut Project one of the largest microbiome studies ever conducted, analyzing data from over 10,000 people found that the number of different plant species a person eats each week is more strongly linked to gut microbial diversity than whether they are vegan, vegetarian, or omnivore. People who regularly ate 30 or more different plant types per week had measurably richer gut communities than those eating fewer than 10 (McDonald et al., mSystems, 2018).
Different plants contain different types of fiber, and different gut bacteria feed on different types. When you eat narrowly, you feed a narrow range of bacteria. When you eat broadly rotating through vegetables, fruits, whole grains, legumes, nuts, seeds, herbs, and spices you feed a much wider and more protective community.
Reaching 30 plant varieties per week is more achievable than it sounds. Herbs and spices count. So do nuts, seeds, and wholegrains. Varying the fruit in your yogurt, tossing a new vegetable into dinner, or adding mixed seeds to breakfast can quickly add up.
2. Make Fermented Foods a Daily Habit
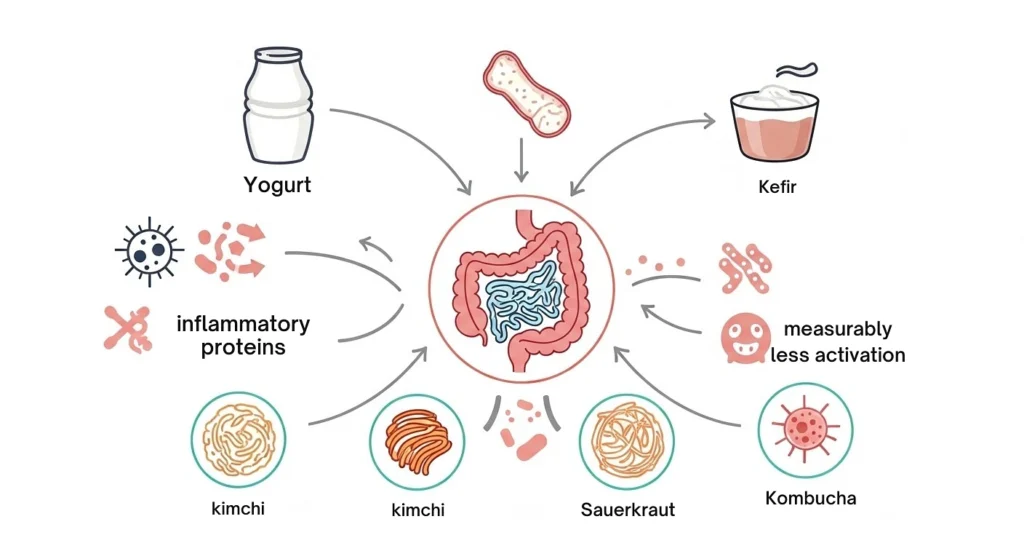
Fermented foods go beyond simple probiotics they can actively reshape inflammation at a measurable level.
In a 17-week randomized controlled trial published in the journal Cell (2021), researchers at Stanford University split 36 healthy adults into two groups one on a high-fermented-food diet, the other on a high-fiber diet. The fermented food group ate yogurt, kefir, kimchi, sauerkraut, and kombucha daily.
At the end of the study, this group showed a clear increase in overall microbial diversity. More significantly for inflammation, 19 inflammatory proteins in the blood decreased, and four types of immune cells showed measurably less activation. These effects held across every participant in the fermented food arm (Wastyk et al., Cell, 2021).
A daily serving of plain yogurt with live cultures, a side of kimchi, or a glass of kefir is a low-cost, evidence-backed way to push back against chronic gut inflammation.
3. Cut Back on Ultra-Processed Foods
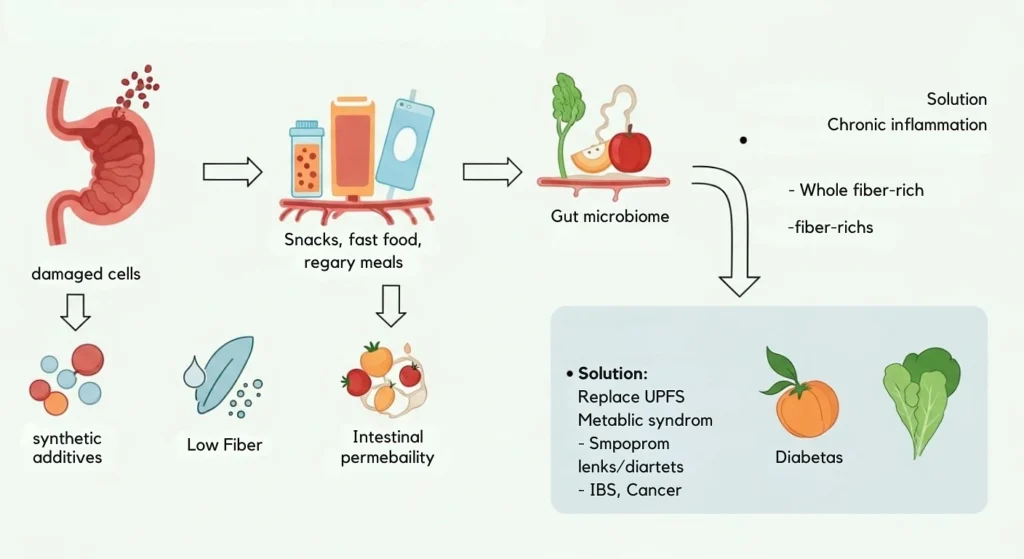
No dietary upgrade matters as much if you are simultaneously feeding your gut the wrong fuel.
Ultra-processed foods (UPFs) packaged snacks, fast food, sugary drinks, ready meals loaded with additives and emulsifiers are among the most consistently damaging forces on the gut microbiome. Their high synthetic additive content and near-zero fiber strip beneficial bacteria, increase intestinal permeability, and fuel chronic inflammation. These microbial shifts have been linked to metabolic syndrome, IBS, type 2 diabetes, and colorectal cancer (Facchin et al., Nutrients, 2025).
You do not need to eliminate every processed food overnight. But steadily replacing UPFs with whole, minimally processed foods and increasing fiber-rich plant variety is one of the most direct anti-inflammatory moves you can make for your gut.
4. Protect Your Sleep
The gut microbiome follows a circadian rhythm, just like the rest of your body. Disrupt the schedule and the microbiome pays the price.
Research published in Scientific Reports (2023) found that just a few nights of severe sleep restriction dropped gut microbial community richness by 21% compared to adequate sleep in healthy young men. A review from the University of Colorado-Boulder also concluded that insufficient sleep and circadian misalignment are associated with adverse metabolic outcomes, with the altered gut microbiome identified as one of the key pathways involved (Depner et al., Current Opinion in Endocrine and Metabolic Research, 2020).
Aim for 7–9 hours per night. Keep a consistent sleep schedule, including weekends, and reduce screen exposure in the evening blue light from screens delays melatonin release, which pushes your circadian rhythm later and disrupts the gut’s natural overnight recovery processes (Karl et al., Scientific Reports, 2023).
5. Move Your Body Consistently
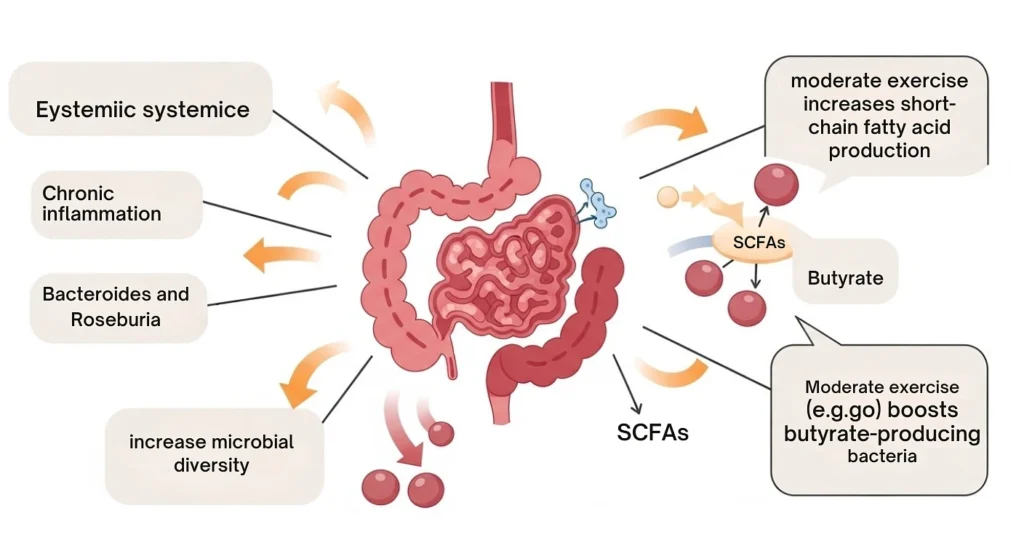
Exercise is good for the gut in ways that are distinct from diet. Physical health activity reduces systemic inflammation, increases intestinal transit time, and directly shifts the microbial community in beneficial ways.
A 2023 systematic review published in Frontiers in Physiology, covering 32 exercise studies across human and animal models, found that regular exercise consistently increased the abundance of Bacteroides and Roseburia two key short-chain fatty acid (SCFA) producers involved in regulating intestinal permeability and glucose metabolism. SCFAs, particularly butyrate, are the primary fuel source for cells lining the colon and are critical for maintaining gut barrier integrity (Cullen, Shahzad & Dhillon, Frontiers in Physiology, 2023).
Women who exercised for at least 3 hours per week showed elevated levels of butyrate-producing bacteria including Faecalibacterium prausnitzii and Akkermansia muciniphila two species most commonly depleted by inflammation. You do not need elite training. Brisk walking, cycling, or swimming practiced consistently shifts the microbial environment in a measurable direction.
6. Manage Stress as a Gut Health Strategy
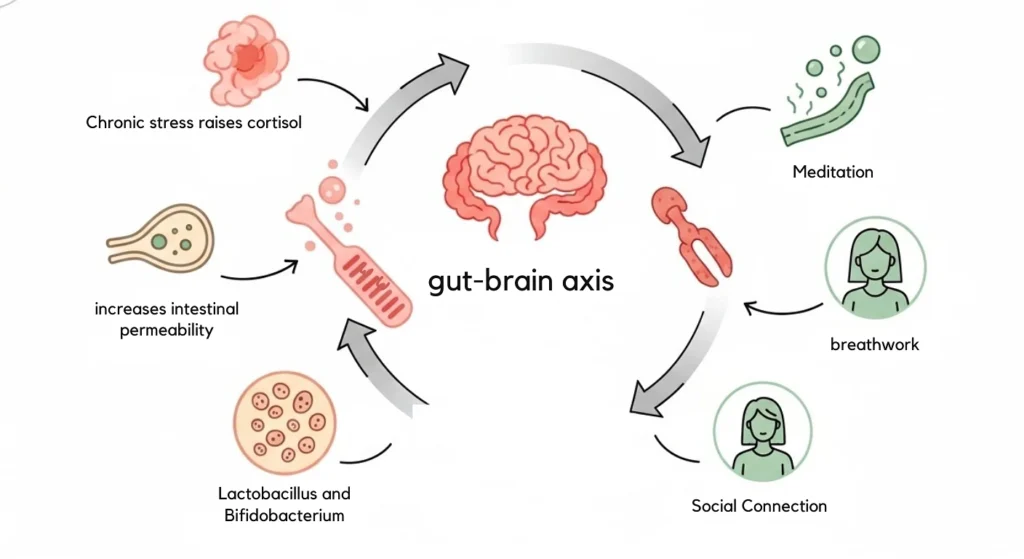
The gut and brain are in constant two-way communication through the gut-brain axis. Your gut produces roughly 90% of the body’s serotonin, and beneficial bacteria like Lactobacillus and Bifidobacterium contribute to the production of serotonin and gamma-aminobutyric acid (GABA) neurotransmitters that regulate mood, anxiety, and sleep.
Chronic stress raises cortisol, increases intestinal permeability, and disrupts microbial balance. The relationship is circular: a disrupted gut makes stress harder to manage, and unmanaged stress disrupts the gut further.
Meditation, breathwork, time in nature, and regular social connection are all practical tools that influence the gut-brain axis in ways that support microbial balance over time. None of them require a prescription. All of them compound their benefit the more consistently they are practiced.
7. Be Strategic About Supplements and Antibiotics
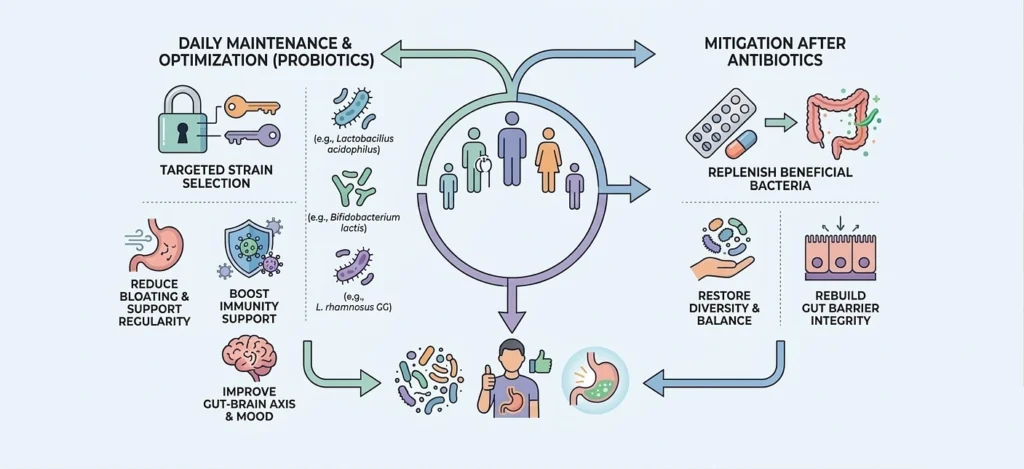
Antibiotic courses are sometimes necessary and life-saving. They are also among the most powerful disruptors of the gut microbiome, wiping out beneficial bacteria alongside the harmful ones. Use antibiotics only when prescribed by a doctor, never for viral infections, and consider reintroducing fermented foods and diverse plant fiber in the weeks that follow to support microbial recovery.
Probiotic supplements can be useful particularly after antibiotic use or acute digestive illness but food-based sources are generally preferred for long-term maintenance and provide a broader range of microbial strains than any single capsule. Consult a healthcare professional before starting any gut-related supplement to ensure the strains and dosages suit your specific situation.
Signs Your Gut Is Responding
As your microbiome becomes healthier and less inflamed, changes tend to show up gradually across several areas: more regular and comfortable digestion, reduced bloating, better energy and mental health clarity, improved mood stability, clearer skin, and fewer colds and infections.
These are not separate outcomes they are all downstream of a more resilient and balanced gut community.
Building gut health is not about one superfood or one supplement. It is the result of consistent daily decisions what you eat, how you sleep, how much you move, how you handle stress compounded over weeks and months into something that genuinely changes how you feel.
References
- McDonald D. et al., “American Gut: an Open Platform for Citizen Science Microbiome Research”, mSystems, 2018 — https://pmc.ncbi.nlm.nih.gov/articles/PMC5954204/
- Wastyk H.C. et al., “Gut-microbiota-targeted diets modulate human immune status”, Cell, 2021; 184(16):4137–4153 — https://pmc.ncbi.nlm.nih.gov/articles/PMC9020749/
- Facchin S. et al., “The Detrimental Impact of Ultra-Processed Foods on the Human Gut Microbiome and Gut Barrier”, Nutrients, 2025 — https://pmc.ncbi.nlm.nih.gov/articles/PMC11901572/
- Karl J.P. et al., “Severe, short-term sleep restriction reduces gut microbiota community richness”, Scientific Reports, 2023; 13:213 — https://www.nature.com/articles/s41598-023-27463-0
- Depner C.M. et al., “Sleep and Circadian Disruption and the Gut Microbiome — Possible Links to Dysregulated Metabolism”, Current Opinion in Endocrine and Metabolic Research, 2020 — https://pmc.ncbi.nlm.nih.gov/articles/PMC8597978/
- Cullen J.M., Shahzad S., Dhillon J., “A systematic review on the effects of exercise on gut microbial diversity, taxonomic composition, and microbial metabolites”, Frontiers in Physiology, 2023 — https://www.frontiersin.org/journals/physiology/articles/10.3389/fphys.2023.1292673/full


